Diseases of the Gallbladder and Bile
Ducts
Physiology of Bile Production and Flow
Bile Secretion and Composition
Bile
formed in the hepatic lobules is secreted into a complex network of canaliculi,
small bile ductules, and larger bile ducts that run with lymphatics and
branches of the portal vein and hepatic artery in portal tracts situated
between hepatic lobules. These interlobular bile ducts coalesce to form larger
septal bile ducts that join to form the right and left hepatic ducts, which in
turn unite to form the common hepatic duct. The common hepatic duct is joined
by the cystic duct of the gallbladder to form the common bile duct (CBD), which
enters the duodenum (often after joining the main pancreatic duct) through the
ampulla of Vater.
Hepatic
bile is an isotonic fluid with an electrolyte composition resembling blood
plasma. The electrolyte composition of gallbladder bile differs from that of
hepatic bile because most of the inorganic anions, chloride and bicarbonate,
have been removed by reabsorption across the gallbladder epithelium.
Major
components of bile by weight include water (82%), bile acids (12%), lecithin
and other phospholipids (4%), and unesterified cholesterol (0.7%). Other
constituents include conjugated bilirubin, proteins (IgA, metabolites of
hormones, and other proteins metabolized in the liver), electrolytes, mucus,
and, often, drugs and their metabolites.
The
total daily basal secretion of hepatic bile is approximately 500 to 600 mL.
Many substances taken up or synthesized by the hepatocyte are secreted into the
bile canalculi. The canalicular membrane forms microvilli and is associated
with microfilaments of actin, microtubules, and other contractile elements.
Prior to their secretion into the bile, many substances that are taken up into
the hepatocyte are conjugated, while others such as phospholipids, a portion of
primary bile acids, and some cholesterol are synthesized de novo in the
hepatocyte. Three mechanisms are important in regulating bile flow: (1) active
transport of bile acids from hepatocytes into the bile canaliculi, (2) active
transport of other organic anions, and (3) cholangiocellular secretion. The
last is a secretin-mediated and cyclic AMP-dependent mechanism that ultimately
results in the secretion of a sodium- and bicarbonate-rich fluid into the bile
ducts.
Active
vectorial secretion of biliary constituents from the portal blood into the bile
canaliculi is driven by a distinct set of polarized transport systems at the
basolateral (sinusoidal) and the canalicular plasma membrane domains of the
hepatocyte. Two sinusoidal bile salt uptake systems have been cloned in humans,
the Na+/taurocholate cotransporter and the organic anion
transporting protein, which also transports a large variety of non-bile salt
organic anions. Four ATP-dependent canalicular transport systems ("export
pumps") have been identified: a bile salt export pump (BSEP), which was
formerly called "sister of P-glycoprotein"; a conjugate export pump
(MRP2), also called the canalicular multispecific organic anion transporter,
which mediates the canalicular excretion of various amphiphilic conjugates
formed by phase II conjugation (e.g., bilirubin diglucuronide); a multidrug
export pump (MDR1) for hydrophobic cationic compounds; and a phospholipid export
pump (MDR3). The canalicular membrane also contains ATP-independent transport
systems such as the Cl-/HCO3- anion exchanger
isoform 2 for canalicular bicarbonate secretion. For some of these
transporters, genetic defects have been identified that are associated with
various forms of cholestasis or defects of biliary excretion. BSEP is defective
in progressive familial intrahepatic cholestasis (PFIC) type 2. Mutations of
MRP2 cause the Dubin-Johnson syndrome, an inherited form of conjugated
hyperbilirubinemia. A defective MDR3 results in PFIC-3. The cystic fibrosis
transmembrane regulator located on bile duct epithelial cells is defective in
cystic fibrosis, which may be associated with impaired cholangiocellular bile
formation and chronic cholestatic liver disease.
The Bile Acids
The
primary bile acids, cholic acid and chenodeoxycholic acid (CDCA), are
synthesized from cholesterol in the liver, conjugated with glycine or taurine,
and excreted into the bile. Secondary bile acids, including deoxycholate and lithocholate,
are formed in the colon as bacterial metabolites of the primary bile acids.
However, lithocholic acid is much less efficiently absorbed from the colon than
deoxycholic acid. Another secondary bile acid, found in low concentration is
ursodeoxycholic acid (UDCA), a stereoisomer of CDCA. In normal bile, the ratio
of glycine to taurine conjugates is about 3:1.
Bile
acids are detergents that in aqueous solutions and above a critical
concentration of about 2 mM form molecular aggregates called micelles.
Cholesterol alone is poorly soluble in aqueous environments, and its solubility
in bile depends on both the total lipid concentration and the relative molar
percentages of bile acids and lecithin. Normal ratios of these constituents
favor the formation of solubilizing mixed micelles, while abnormal
ratios promote the precipitation of cholesterol crystals in bile.
In
addition to facilitating the biliary excretion of cholesterol, bile acids are
necessary for the normal intestinal absorption of dietary fats via a micellar
transport mechanism (Chap. 286). Bile acids also serve as a major physiologic
driving force for hepatic bile flow and aid in water and electrolyte transport
in the small bowel and colon.
Enterohepatic Circulation
Bile
acids are efficiently conserved under normal conditions. Unconjugated, and to a
lesser degree also conjugated, bile acids are absorbed by passive diffusion
along the entire gut. Quantitatively much more important for bile salt
recirculation, however, is the active transport mechanism for conjugated
bile acids in the distal ileum (Chap. 286). The reabsorbed bile acids enter the
portal bloodstream and are taken up rapidly by hepatocytes, reconjugated, and
resecreted into bile (enterohepatic circulation).
The
normal bile acid pool size is approximately 2 to 4 g. During digestion of a
meal, the bile acid pool undergoes at least one or more enterohepatic cycles,
depending on the size and composition of the meal. Normally, the bile acid pool
circulates approximately 5 to 10 times daily. Intestinal absorption of the pool
is about 95% efficient, so fecal loss of bile acids is in the range of 0.3 to
0.6 g/d. This fecal loss is compensated by an equal daily synthesis of bile
acids by the liver, and thus the size of the bile acid pool is maintained. Bile
acids returning to the liver suppress de novo hepatic synthesis of primary bile
acids from cholesterol by inhibiting the rate-limiting enzyme cholesterol 7![]() -hydroxylase.
While the loss of bile salts in stool is usually matched by increased hepatic
synthesis, the maximum rate of synthesis is approximately 5 g/d, which may be
insufficient to replete the bile acid pool size when there is pronounced
impairment of intestinal bile salt reabsorption.
-hydroxylase.
While the loss of bile salts in stool is usually matched by increased hepatic
synthesis, the maximum rate of synthesis is approximately 5 g/d, which may be
insufficient to replete the bile acid pool size when there is pronounced
impairment of intestinal bile salt reabsorption.
Gallbladder and Sphincteric Functions
In
the fasting state, the sphincter of Oddi offers a high-pressure zone of
resistance to bile flow from the common bile duct into the duodenum. This tonic
contraction serves to (1) prevent reflux of duodenal contents into the
pancreatic and bile ducts and (2) promote bile filling of the gallbladder. The
major factor controlling the evacuation of the gallbladder is the peptide hormone
cholecystokinin (CCK), which is released from the duodenal mucosa in response
to the ingestion of fats and amino acids. CCK produces (1) powerful contraction
of the gallbladder, (2) decreased resistance of the sphincter of Oddi, (3)
increased hepatic secretion of bile, and thus (4) enhanced flow of biliary
contents into the duodenum.
Hepatic
bile is "concentrated" within the gallbladder by energy-dependent
transmucosal absorption of water and electrolytes. Almost the entire bile acid
pool may be sequestered in the gallbladder following an overnight fast for
delivery into the duodenum with the first meal of the day. The normal capacity
of the gallbladder is 30 to 50 mL of bile.
Diseases of the Gallbladder
Congenital Anomalies
Anomalies
of the biliary tract may be found in 10 to 20% of the population, including
abnormalities in number, size, and shape (e.g., agenesis of the gallbladder,
duplications, rudimentary or oversized "giant" gallbladders, and
diverticula). Phrygian cap is a clinically innocuous entity in which a partial
or complete septum (or fold) separates the fundus from the body. Anomalies of
position or suspension are not uncommon and include left-sided gallbladder,
intrahepatic gallbladder, retrodisplacement of the gallbladder, and
"floating" gallbladder. The latter condition predisposes to acute
torsion, volvulus, or herniation of the gallbladder.
Gallstones
Pathogenesis
Gallstones
are quite prevalent in most western countries. In the United States, autopsy
series have shown gallstones in at least 20% of women and in 8% of men over the
age of 40. It is estimated that 16 to 20 million persons in the United States
have gallstones and that approximately 1 million new cases of cholelithiasis
develop each year.
Gallstones
are formed by concretion or accretion of normal or abnormal bile constituents.
They are divided into three major types; cholesterol and mixed stones account
for 80% of the total, with pigment stones comprising the remaining 20%. Mixed
and cholesterol gallstones usually contain more than 50% cholesterol
monohydrate plus an admixture of calcium salts, bile pigments, proteins, and
fatty acids. Pigment stones are composed primarily of calcium bilirubinate;
they contain less than 20% cholesterol.
Cholesterol and Mixed Stones and Biliary Sludge
Cholesterol
is essentially water insoluble and requires aqueous dispersion into either
micelles or vesicles, both of which require the presence of a second lipid to
"liquefy" the cholesterol. Cholesterol and phospholipids are secreted
into bile as unilamellar bilayered vesicles, which are converted into mixed
micelles consisting of bile acids, phospholipids, and cholesterol by the action
of bile acids. If there is an excess of cholesterol in relation to
phospholipids and bile acids, unstable cholesterol-rich vesicles remain, which
aggregate into large multilamellar vesicles from which cholesterol crystals
precipitate (Fig. 302-1).
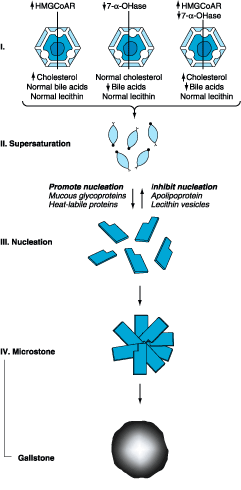
Figure 302-1: Scheme showing pathogenesis of gallstone
formation. Conditions or factors that increase the ratio of cholesterol to bile
acids and lecithin favor gallstone formation (HMG-CoAR,
hydroxymethylglutaryl-coenzyme A reductase; 7-![]() -OHase,
cholesterol, 7
-OHase,
cholesterol, 7![]() -hydroxylase).
-hydroxylase).
There
are several important mechanisms in the formation of lithogenic (stone-forming)
bile. The most important is increased biliary secretion of cholesterol. This
may occur in association with obesity, high-caloric and cholesterol-rich diets,
or drugs (e.g., clofibrate) and may result from increased activity of HMG-CoA
reductase, the rate-limiting enzyme of hepatic cholesterol synthesis, and
increased hepatic uptake of cholesterol from blood. In patients with gallstones,
dietary cholesterol increases biliary cholesterol secretion. This does
not occur in non-gallstone patients on high-cholesterol diets. In addition to
environmental factors such as high-caloric and cholesterol-rich diets, genetic
factors play an important role in cholesterol hypersecretion and gallstone
formation. A high prevalence of gallstones is found among first-degree
relatives of gallstone carriers and in certain ethnic populations such as
American Indians as well as Chilean Indians and Chilean Hispanics. A common
genetic trait has been identified for some of these populations by
mitochondrial DNA analysis. A genetic defect in the control of cholesterol
secretion also exists in certain strains of inbred mice who develop gallstones
under a lithogenic diet. In some patients, impaired hepatic conversion of
cholesterol to bile acids may also occur, resulting in an increase of the
lithogenic cholesterol/bile acid ratio. Lithogenic bile may also result from
conditions affecting the enterohepatic circulation of bile acids (e.g.,
prolonged parenteral alimentation or ileal disease or resection). In addition,
most patients with gallstones may have reduced activity of hepatic cholesterol
7![]() -hydroxylase,
the rate-limiting enzyme for primary bile acid synthesis.
-hydroxylase,
the rate-limiting enzyme for primary bile acid synthesis.
Thus
an excess of biliary cholesterol in relation to bile acids and phospholipids is
primarily due to hypersecretion of cholesterol, but hyposecretion of bile acids
may contribute. Two additional disturbances of bile acid metabolism that are
likely to contribute to supersaturation of bile with cholesterol are (1)
reduction of the bile acid pool and (2) enhanced conversion of cholic acid to
deoxycholic acid, with replacement of the cholic acid pool by an expanded
deoxycholic acid pool. The first disorder may be caused by more rapid loss of
primary bile acid from the small intestine into the colon. The second
disturbance may result from enhanced dehydroxylation of cholic acid and
increased absorption of newly formed deoxycholic acid. An increased
deoxycholate secretion is associated with hypersecretion of cholesterol into
bile. While supersaturation of bile with cholesterol is an important
prerequisite for gallstone formation, it is not sufficient by itself to produce
cholesterol precipitation in vivo. Most people with supersaturated bile do not
develop stones because the time required for cholesterol crystals to nucleate
and grow is longer than the time bile spends in the gallbladder.
A
second important mechanism is nucleation of cholesterol monohydrate
crystals, which is greatly accelerated in human lithogenic bile; it is this
feature rather than the degree of cholesterol supersaturation that
distinguishes lithogenic from normal gallbladder bile. Accelerated nucleation
of cholesterol monohydrate in bile may be due to either an excess of
pronucleating factors or a deficiency of antinucleating factors.
Mucin and certain non-mucin glycoproteins appear to be pronucleating factors,
while apolipoproteins AI and AII and other glycoproteins appear to be
antinucleating factors. Cholesterol monohydrate crystal nucleation and crystal
growth probably occur within the mucin gel layer. Vesicle fusion leads to
liquid crystals, which, in turn, nucleate into solid cholesterol monohydrate
crystals. Continued growth of the crystals occurs by direct nucleation of
cholesterol molecules from supersaturated unilamellar or multilamellar biliary
vesicles.
A
third important mechanism in cholesterol gallstone formation is gallbladder
hypomotility. If the gallbladder emptied all supersaturated or
crystal-containing bile completely, stones would not be able to grow. A high
percentage of patients with gallstones exhibits abnormalities of gallbladder
emptying. Ultrasonographic studies show that gallstone patients have an
increased gallbladder volume during fasting and also after a test meal
(residual volume) and that fractional emptying after gallbladder stimulation is
decreased. Gallbladder emptying is a major determinant of gallstone recurrence
in patients who underwent biliary lithotripsy. Within 3 years, only 13% of
patients with good but 53% of patients with poor gallbladder emptying form
recurrent stones.
Biliary
sludge is a thick mucous material that upon microscopic examination reveals
lecithin-cholesterol crystals, cholesterol monohydrate crystals, calcium
bilirubinate, and mucin thread or mucous gels. Biliary sludge typically forms a
crescent-like layer in the most dependent portion of the gallbladder and is
recognized by characteristic echoes on ultrasonography (see below). The
presence of biliary sludge implies two abnormalities: (1) the normal balance
between gallbladder mucin secretion and elimination has become deranged and (2)
nucleation of biliary solutes has occurred. That biliary sludge may be a
precursor form of gallstone disease is evident from several observations. In
one study, 96 patients with gallbladder sludge were followed prospectively by serial
ultrasound studies. In 18%, biliary sludge disappeared and did not recur for at
least 2 years. In 60%, biliary sludge disappeared and reappeared; in 14%,
gallstones (8% asymptomatic, 6% symptomatic) developed, and in 6%, severe
biliary pain with or without acute pancreatitis occurred. In 12 patients,
cholecystectomies were performed, 6 for gallstone-associated biliary pain and 3
in symptomatic patients with sludge but without gallstones who had prior
attacks of pancreatitis; the latter did not recur after cholecystectomy. It
should be emphasized that biliary sludge can develop with disorders that cause
gallbladder hypomotility, i.e., surgery, burns, total parenteral nutrition,
pregnancy, and oral contraceptives-all of which are associated with gallstone
formation.
Two
other conditions are associated with cholesterol stone or biliary sludge
formation: pregnancy and very low calorie diet. There appear to be two key
changes during pregnancy that contribute to a "cholelithogenic
state." First, the composition of the bile acid pool and the
cholesterol-carrying capacity of bile change, with a resultant marked increase
in cholesterol saturation during the third trimester. Second, ultrasonographic
studies have demonstrated that gallbladder contraction in response to a
standard meal is sluggish, resulting in impaired gallbladder emptying. That
these changes are related to pregnancy per se is supported by several studies
that show reversal of these abnormalities after delivery. During pregnancy,
gallbladder sludge develops in 20 to 30% of women and gallstones in 5 to 12%.
While biliary sludge is a common finding during pregnancy, it is usually
asymptomatic and often resolves spontaneously after delivery. Gallstones, which
are less common than sludge and frequently associated with biliary colic, may
also disappear after delivery because of spontaneous dissolution related to
bile becoming unsaturated with cholesterol post partum.
From
10 to 20% of people having rapid weight reduction through very low calorie
dieting develop gallstones. In a study involving 600 patients who completed a
16-week, 520-kcal/d diet, UDCA in a dosage of 600 mg/d proved highly effective
in preventing gallstone formation; gallstones developed in only 3% of UDCA
recipients compared to 28% of placebo-treated patients.
To
summarize, cholesterol gallstone disease occurs because of several defects,
which include (1) bile supersaturation with cholesterol, (2) nucleation of
cholesterol monohydrate with subsequent crystal retention and stone growth, and
(3) abnormal gallbladder motor function with delayed emptying and stasis. Other
important factors known to predispose to cholesterol stone formation are
summarized in Table 302-1.
Table 302-1: Predisposing Factors for
Cholesterol and Pigment Gallstone Formation
|
Pigment Stones
Gallstones
composed largely of calcium bilirubinate are much more common in the Far East
than in western countries. The presence of increased amounts of unconjugated,
insoluble bilirubin in bile results in the precipitation of bilirubin, which
may aggregate to form pigment stones or may form the nidus for growth of mixed
cholesterol gallstones. In western countries, chronic hemolytic states (with
increased conjugated bilirubin in bile) or alcoholic liver disease are
associated with an increased incidence of pigment stones. Deconjugation of an
excess of soluble bilirubin mono- and diglucuronide may be mediated by
endogenous ![]() -glucuronidase
but may also occur by spontaneous alkaline hydrolysis. Sometimes, the enzyme is
also produced when bile is chronically infected by bacteria. Pigment stone
formation is especially prominent in Asians and is often associated with
infections in the biliary tree (Table 302-1).
-glucuronidase
but may also occur by spontaneous alkaline hydrolysis. Sometimes, the enzyme is
also produced when bile is chronically infected by bacteria. Pigment stone
formation is especially prominent in Asians and is often associated with
infections in the biliary tree (Table 302-1).
Diagnosis
Procedures
of potential use in the diagnosis of cholelithiasis and other diseases of the
gallbladder are detailed in Table 302-2. The plain abdominal film may detect
gallstones containing sufficient calcium to be radiopaque (10 to 15% of
cholesterol and mixed stones and approximately 50% of pigment stones). Plain
radiography may also be of use in the diagnosis of emphysematous cholecystitis,
porcelain gallbladder, limey bile, and gallstone ileus.
Table 302-2: Diagnostic Evaluation of the
Gallbladder
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
Ultrasonography
of the gallbladder is very accurate in the identification of cholelithiasis and
has several advantages over oral cholecystography (Fig. 302-2A). The
gallbladder is easily visualized with the technique, and in fact, failure to image
the gallbladder successfully in a fasting patient correlates well with the
presence of underlying gallbladder disease. Stones as small as 2 mm in diameter
may be confidently identified provided that firm criteria are used [e.g.,
acoustic "shadowing" of opacities that are within the gallbladder
lumen and that change with the patient's position (by gravity)]. In major
medical centers, the false-negative and false-positive rates for ultrasound in
gallstone patients are about 2 to 4%. Biliary sludge is material of low
echogenic activity that typically forms a layer in the most dependent position
of the gallbladder. This layer shifts with postural changes but fails to
produce acoustic shadowing; these two characteristics distinguish sludges from
gallstones. Ultrasound can also be used to assess the emptying function of the
gallbladder.
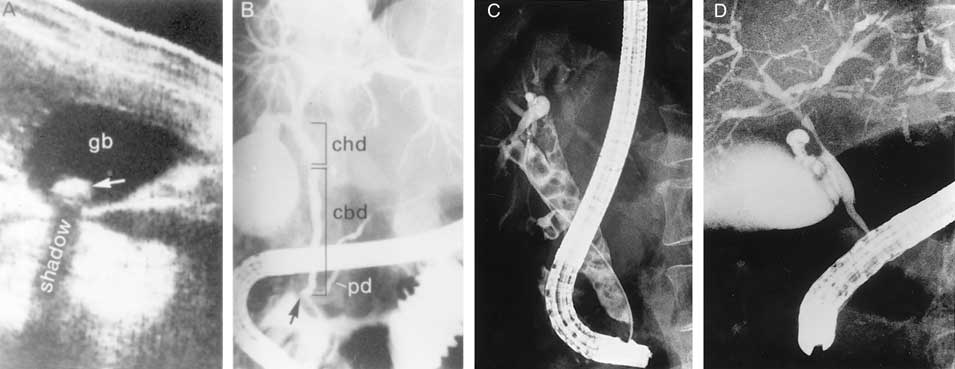
Figure 302-2: Examples of ultrasound and radiologic studies
of the biliary tract. A. An ultrasound study showing a distended
gallbladder containing a single large stone (arrow) which casts an
acoustic shadow. B. Endoscopic retrograde cholangiopancreatogram (ERCP)
showing normal biliary tract anatomy. In addition to the endoscope and large
vertical gallbladder filled with contrast dye, the common hepatic duct (chd),
common bile duct (cbd), and pancreatic duct (pd) are shown. The arrow points to
the ampulla of Vater. C. Percutaneous transhepatic cholangiogram (PTHC)
showing choledocholithiasis. The biliary tract is dilatated and contains
multiple radiolucent calculi. D. ERCP showing sclerosing cholangitis.
The common bile duct shows areas that are strictured and narrowed.
Oral
cholecystography (OCG) is a useful procedure for the diagnosis of gallstones
but has been largely replaced by ultrasound. However, OCG is still useful for
the selection of patients for nonsurgical therapy of gallstone disease such as
lithotripsy or bile acid dissolution therapy. In both these settings, OCG is
used to assess the patency of the cystic duct and gallbladder emptying
function. Further, OCG can also delineate the size and number of gallstones and
determine whether they are calcified. Factors that may produce nonvisualization
of the OCG are summarized in Table 302-2.
Radiopharmaceuticals
such as 99mTc-labeled N-substituted iminodiacetic acids
(HIDA, DIDA, DISIDA, etc.) are rapidly extracted from the blood and are
excreted into the biliary tree in high concentration even in the presence of
mild to moderate serum bilirubin elevations. Failure to image the gallbladder
in the presence of biliary ductal visualization may indicate cystic duct
obstruction, acute or chronic cholecystitis, or surgical absence of the organ.
Such scans have their greatest application in the diagnosis of acute
cholecystitis.
Symptoms of Gallstone Disease
Gallstones
usually produce symptoms by causing inflammation or obstruction following their
migration into the cystic duct or CBD. The most specific and characteristic
symptom of gallstone disease is biliary colic. Obstruction of the cystic duct
or CBD by a stone produces increased intraluminal pressure and distention of
the viscus that cannot be relieved by repetitive biliary contractions. The
resultant visceral pain is characteristically a severe, steady ache or pressure
in the epigastrium or right upper quadrant (RUQ) of the abdomen with frequent
radiation to the interscapular area, right scapula, or shoulder.
Biliary
colic begins quite suddenly and may persist with severe intensity for 30 min to
5 h, subsiding gradually or rapidly. An episode of biliary pain is sometimes
followed by a residual mild ache or soreness in the RUQ, which may persist for
24 h or so. Nausea and vomiting frequently accompany episodes of biliary colic.
An elevated level of serum bilirubin and/or alkaline phosphatase suggests a
common duct stone. Fever or chills (rigors) with biliary colic usually imply a
complication, i.e., cholecystitis, pancreatitis, or cholangitis. Complaints of
vague epigastric fullness, dyspepsia, eructation, or flatulence, especially
following a fatty meal, should not be confused with biliary colic. Such
symptoms are frequently elicited from patients with gallstone disease but are
not specific for biliary calculi. Biliary colic may be precipitated by eating a
fatty meal, by consumption of a large meal following a period of prolonged
fasting, or by eating a normal meal.
Natural History
Gallstone
disease discovered in an asymptomatic patient or in a patient whose symptoms
are not referable to cholelithiasis is a common clinical problem. The natural
history of "silent" or asymptomatic gallstones has occasioned much
debate. A study of predominantly male silent gallstone patients suggests that
the cumulative risk for the development of symptoms or complications requiring
surgery is relatively low-10% at 5 years, 15% at 10 years, and 18% at 15 years.
Patients remaining asymptomatic for 15 years were found to be unlikely to
develop symptoms during further follow-up, and most patients who did develop
complications from their gallstones experienced prior warning symptoms.
Similar conclusions apply to diabetic patients with silent gallstones. Decision
analysis has suggested that (1) the cumulative risk of death due to gallstone
disease while on expectant management is small, and (2) prophylactic
cholecystectomy is not warranted.
Complications
requiring cholecystectomy are much more common in gallstone patients who have
developed symptoms of biliary colic. Patients found to have gallstones at a
young age are more likely to develop symptoms from cholelithiasis than are
patients older than 60 years at the time of initial diagnosis. Patients with
diabetes mellitus and gallstones may be somewhat more susceptible to septic
complications, but the magnitude of risk of septic biliary complications in
diabetic patients is incompletely defined. In addition, asymptomatic gallstone
patients with nonvisualization of the gallbladder on OCG appear to have an
increased tendency to develop symptoms and complications.
![]() Treatment
Treatment
Surgical Therapy
In
asymptomatic gallstone patients, the risk of developing symptoms or
complications requiring surgery is quite small (in the range of 1 to 2% per
year). Thus a recommendation for cholecystectomy in a patient with gallstones
should probably be based on assessment of three factors: (1) the presence of
symptoms that are frequent enough or severe enough to interfere with the
patient's general routine; (2) the presence of a prior complication of
gallstone disease, i.e., history of acute cholecystitis, pancreatitis,
gallstone fistula, etc.; or (3) the presence of an underlying condition
predisposing the patient to increased risk of gallstone complications (e.g.,
calcified or porcelain gallbladder and/or a previous attack of acute
cholecystitis regardless of current symptomatic status). Patients with very
large gallstones (over 2 cm in diameter) and patients having gallstones in a
congenitally anomalous gallbladder might also be considered for prophylactic
cholecystectomy. Although age under 50 years is a worrisome factor in
asymptomatic gallstone patients, few authorities would now recommend routine
cholecystectomy in all young patients with silent stones. Laparoscopic
cholecystectomy is a minimal-access approach for the removal of the gallbladder
together with its stones. Its advantages include a markedly shortened hospital
stay as well as decreased cost, and it is the procedure of choice for most
patients referred for elective cholecystectomy.
From
several studies involving over 4000 patients undergoing laparoscopic
cholecystectomy, the following key points emerge: (1) complications develop in
about 4% of patients, (2) conversion to laparotomy occurs in 5%, (3) the death
rate is remarkably low (i.e., <0.1%), and (4) bile duct injuries are unusual
(i.e., 0.2 to 0.5%). These data indicate why laparoscopic cholecystectomy has
become the "gold standard" for treating symptomatic cholelithiasis.
Medical Therapy-Gallstone Dissolution
UDCA
decreases cholesterol saturation of bile and also appears to produce a lamellar
liquid crystalline phase in bile that allows a dispersion of cholesterol from
stones by physiochemical means. UDCA may also retard cholesterol crystal
nucleation. In carefully selected patients with a functioning gallbladder and
with radiolucent stones <10 mm in diameter, complete dissolution can be
achieved in about 50% of patients within 6 months to 2 years with UDCA at a
dose of 8 to 10 mg/kg per day. The highest success rate (i.e., >70%) occurs
in patients with small (<5 mm) floating radiolucent gallstones. Probably no
more than 10% of patients with symptomatic cholelithiasis are candidates
for such treatment. However, in addition to the vexing problem of recurrent
stones (30 to 50% over 3 to 5 years of follow-up), there is also the factor of
taking an expensive drug for an indefinite period of time. The advantages and
success of laparoscopic cholecystectomy have largely reduced the role of
gallstone dissolution to patients who wish to avoid or are not candidates for
elective cholecystectomy.
Gallbladder
stones may be fragmented by extracorporeal shock waves. While such shock wave
lithotripsy combined with medical litholytic therapy is safe and effective in
carefully selected patients with gallbladder calculi (radiolucent, solitary
stone <2 cm in well-contracting gallbladder), the procedure is employed
infrequently because of the emergence of laparoscopic cholystectomy as the
procedure of choice for symptomatic cholelithiasis, the recurrence of
gallstones in 30% of patients within 5 years after lithotripsy combined with
medical litholytic therapy, and the cost of taking UDCA for a variable period
after the procedure.
Acute and Chronic Cholecystitis
Acute Cholecystitis
Acute
inflammation of the gallbladder wall usually follows obstruction of the cystic
duct by a stone. Inflammatory response can be evoked by three factors: (1) mechanical
inflammation produced by increased intraluminal pressure and distention
with resulting ischemia of the gallbladder mucosa and wall, (2) chemical
inflammation caused by the release of lysolecithin (due to the action of
phospholipase on lecithin in bile) and other local tissue factors, and (3) bacterial
inflammation, which may play a role in 50 to 85% of patients with acute
cholecystitis. The organisms most frequently isolated by culture of gallbladder
bile in these patients include Escherichia coli, Klebsiella spp.,
group D Streptococcus, Staphylococcus spp., and Clostridium
spp.
Acute
cholecystitis often begins as an attack of biliary colic that progressively
worsens. Approximately 60 to 70% of patients report having experienced prior
attacks that resolved spontaneously. As the episode progresses, however, the
pain of acute cholecystitis becomes more generalized in the right upper
abdomen. As with biliary colic, the pain of cholecystitis may radiate to the
interscapular area, right scapula, or shoulder. Peritoneal signs of inflammation
such as increased pain with jarring or on deep respiration may be apparent. The
patient is anorectic and often nauseated. Vomiting is relatively common and may
produce symptoms and signs of vascular and extracellular volume depletion.
Jaundice is unusual early in the course of acute cholecystitis but may occur
when edematous inflammatory changes involve the bile ducts and surrounding
lymph nodes.
A
low-grade fever is characteristically present, but shaking chills or rigors are
not uncommon. The RUQ of the abdomen is almost invariably tender to palpation.
An enlarged, tense gallbladder is palpable in one-quarter to one-half of
patients. Deep inspiration or cough during subcostal palpation of the RUQ
usually produces increased pain and inspiratory arrest (Murphy's sign). A light
blow delivered to the right subcostal area may elicit a marked increase in
pain. Localized rebound tenderness in the RUQ is common, as are abdominal
distention and hypoactive bowel sounds from paralytic ileus, but generalized peritoneal
signs and abdominal rigidity are usually lacking, absent perforation.
The
diagnosis of acute cholecystitis is usually made on the basis of a
characteristic history and physical examination. The triad of sudden onset of
RUQ tenderness, fever, and leukocytosis is highly suggestive. Typically,
leukocytosis in the range of 10,000 to 15,000 cells per microliter with a left
shift on differential count is found. The serum bilirubin is mildly elevated
[<85.5 ![]() mol/L
(5 mg/dL)] in 45% of patients, while 25% have modest elevations in serum
aminotransferases (usually less than a fivefold elevation). The radionuclide
(e.g., HIDA) biliary scan may be confirmatory if bile duct imaging is seen
without visualization of the gallbladder. Ultrasound will demonstrate calculi
in 90 to 95% of cases.
mol/L
(5 mg/dL)] in 45% of patients, while 25% have modest elevations in serum
aminotransferases (usually less than a fivefold elevation). The radionuclide
(e.g., HIDA) biliary scan may be confirmatory if bile duct imaging is seen
without visualization of the gallbladder. Ultrasound will demonstrate calculi
in 90 to 95% of cases.
Approximately
75% of patients treated medically have remission of acute symptoms within 2 to
7 days following hospitalization. In 25%, however, a complication of acute
cholecystitis will occur despite conservative treatment (see below). In this
setting, prompt surgical intervention is required. Of the 75% of patients with
acute cholecystitis who undergo remission of symptoms, approximately
one-quarter will experience a recurrence of cholecystitis within 1 year, and
60% will have at least one recurrent bout within 6 years. In view of the
natural history of the disease, acute cholecystitis is best treated by early
surgery whenever possible.
Acalculous Cholecystitis
In
5 to 10% of patients with acute cholecystitis, calculi obstructing the cystic
duct are not found at surgery. In over 50% of such cases, an underlying
explanation for acalculous inflammation is not found. An increased risk for the
development of acalculous cholecystitis is especially associated with serious
trauma or burns, with the postpartum period following prolonged labor, and with
orthopedic and other nonbiliary major surgical operations in the postoperative
period. Other precipitating factors include vasculitis, obstructing
adenocarcinoma of the gallbladder, diabetes mellitus, torsion of the
gallbladder, "unusual" bacterial infections of the gallbladder (e.g.,
Leptospira, Streptococcus, Salmonella, or Vibrio
cholerae), and parasitic infestation of the gallbladder. Acalculous
cholecystitis may also be seen with a variety of other systemic disease
processes (sarcoidosis, cardiovascular disease, tuberculosis, syphilis,
actinomycosis, etc.) and may possibly complicate periods of prolonged
parenteral hyperalimentation.
Although
the clinical manifestations of acalculous cholecystitis are indistinguishable
from those of calculous cholecystitis, the setting of acute gallbladder
inflammation complicating severe underlying illness is characteristic of
acalculous disease. Ultrasound, computed tomography (CT) scanning, or
radionuclide examinations demonstrating a large, tense, static gallbladder
without stones and with evidence of poor emptying over a prolonged period may
be diagnostically useful in some cases. The complication rate for acalculous
cholecystitis exceeds that for calculous cholecystitis. Successful management
of acute acalculous cholecystitis appears to depend primarily on early diagnosis
and surgical intervention, with meticulous attention to postoperative care.
Acalculous Cholecystopathy
Disordered
motility of the gallbladder can produce recurrent biliary pain in patients
without gallstones. Infusion of an octapeptide of CCK can be used to measure
the gallbladder ejection fraction during cholescintigraphy. In a representative
study, CCK cholescintigraphy using 99mTc-diisopropyl iminodiacetic
acid (DIDA) identified 21 patients with an abnormal gallbladder ejection
fraction (<40% at 45 min); 10 of 11 patients who underwent surgery became
asymptomatic; all 10 showed abnormalities, i.e., chronic cholecystitis,
gallbladder muscle hypertrophy, and/or a markedly narrowed cystic duct. From
this and other similar studies, the following criteria can be used to identify
patients with acalculous cholecystopathy: (1) recurrent episodes of typical RUQ
pain characteristic of biliary tract pain, (2) abnormal CCK cholescintigraphy
demonstrating a gallbladder ejection fraction of less than 40%, and (3)
infusion of CCK reproduces the patient's pain. An additional clue would be the
identification of a large gallbladder on ultrasound examination. Finally, it
should be noted that sphincter of Oddi dysfunction can also give rise to
recurrent RUQ pain and CCK-scintigraphic abnormalities.
Emphysematous Cholecystitis
So-called
emphysematous cholecystitis is thought to begin with acute cholecystitis
(calculous or acalculous) followed by ischemia or gangrene of the gallbladder
wall and infection by gas-producing organisms. Bacteria most frequently
cultured in this setting include anaerobes, such as C. welchii or C.
perfringens, and aerobes, such as E. coli. This condition occurs
most frequently in elderly men and in patients with diabetes mellitus. The
clinical manifestations are essentially indistinguishable from those of
nongaseous cholecystitis. The diagnosis is usually made on plain abdominal film
by the finding of gas within the gallbladder lumen, dissecting within the
gallbladder wall to form a gaseous ring, or in the pericholecystic tissues. The
morbidity and mortality rates with emphysematous cholecystitis are
considerable. Prompt surgical intervention coupled with appropriate antibiotics
is mandatory.
Chronic Cholecystitis
Chronic
inflammation of the gallbladder wall is almost always associated with the
presence of gallstones and is thought to result from repeated bouts of subacute
or acute cholecystitis or from persistent mechanical irritation of the
gallbladder wall. The presence of bacteria in the bile occurs in more than
one-quarter of patients with chronic cholecystitis. Although the presence of
infected bile in a patient with chronic cholecystitis undergoing
elective cholecystectomy probably adds little to the operative risk,
intraoperative Gram's staining and routine culturing of bile have been
advocated to identify those patients whose gallbladder is colonized with Clostridium
spp. Appropriate antibiotics intra- and postoperatively are recommended in such
patients because colonization with these organisms may be associated with
devastating septic complications following surgery. Chronic cholecystitis may
be asymptomatic for years, may progress to symptomatic gallbladder disease or
to acute cholecystitis, or may present with complications (see below).
Complications of Cholecystitis
Empyema and Hydrops
Empyema
of the gallbladder usually results from progression of acute cholecystitis with
persistent cystic duct obstruction to superinfection of the stagnant bile with
a pus-forming bacterial organism. The clinical picture resembles that of
cholangitis with high fever, severe RUQ pain, marked leukocytosis, and often,
prostration. Empyema of the gallbladder carries a high risk of gram-negative
sepsis and/or perforation. Emergency surgical intervention with proper
antibiotic coverage is required as soon as the diagnosis is suspected.
Hydrops
or mucocele of the gallbladder may also result from prolonged obstruction of
the cystic duct, usually by a large solitary calculus. In this instance, the
obstructed gallbladder lumen is progressively distended, over a period of time,
by mucus (mucocele) or by a clear transudate (hydrops) produced by mucosal
epithelial cells. A visible, easily palpable, nontender mass sometimes
extending from the RUQ into the right iliac fossa may be found on physical
examination. The patient with hydrops of the gallbladder frequently remains
asymptomatic, although chronic RUQ pain may also occur. Cholecystectomy is
indicated, since empyema, perforation, or gangrene may complicate the condition.
Gangrene and Perforation
Gangrene
of the gallbladder results from ischemia of the wall and patchy or complete
tissue necrosis. Underlying conditions often include marked distention of the
gallbladder, vasculitis, diabetes mellitus, empyema, or torsion resulting in
arterial occlusion. Gangrene usually predisposes to perforation of the
gallbladder, but perforation may also occur in chronic cholecystitis without
premonitory warning symptoms. Localized perforations are usually
contained by the omentum or by adhesions produced by recurrent inflammation of
the gallbladder. Bacterial superinfection of the walled-off gallbladder
contents results in abscess formation. Most patients are best treated with
cholecystectomy, but some seriously ill patients may be managed with
cholecystostomy and drainage of the abscess. Free perforation is less
common but is associated with a mortality rate of approximately 30%. Such
patients may experience a sudden transient relief of RUQ pain as the distended
gallbladder decompresses; this is followed by signs of generalized peritonitis.
Fistula Formation and Gallstone Ileus
Fistulization into an adjacent organ adherent to the
gallbladder wall may result from inflammation and adhesion formation. Fistulas
into the duodenum are most common, followed in frequency by those involving the
hepatic flexure of the colon, stomach or jejunum, abdominal wall, and renal
pelvis. Clinically "silent" biliary-enteric fistulas occurring as a
complication of chronic cholecystitis have been found in up to 5% of patients
undergoing cholecystectomy. Asymptomatic cholecystoenteric fistulas may
sometimes be diagnosed by finding gas in the biliary tree on plain abdominal
films. Barium contrast studies or endoscopy of the upper gastrointestinal tract
or colon may demonstrate the fistula. Treatment in the symptomatic patient
usually consists of cholecystectomy, CBD exploration, and closure of the
fistulous tract.
Gallstone ileus refers to mechanical intestinal obstruction
resulting from the passage of a large gallstone into the bowel lumen. The stone
customarily enters the duodenum through a cholecystoenteric fistula at that
level. The site of obstruction by the impacted gallstone is usually at the
ileocecal valve, provided that the more proximal small bowel is of normal
caliber. The majority of patients do not give a history of either prior biliary
tract symptoms or complaints suggestive of acute cholecystitis or
fistulization. Large stones over 2.5 cm in diameter are thought to predispose
to fistula formation by gradual erosion through the gallbladder fundus.
Diagnostic confirmation may occasionally be found on the plain abdominal film
(e.g., small-intestinal obstruction with gas in the biliary tree and a
calcified, ectopic gallstone) or following an upper gastrointestinal series
(cholecystoduodenal fistula with small-bowel obstruction at the ileocecal
valve). Laparotomy with stone extraction (or propulsion into the colon) remains
the procedure of choice to relieve obstruction. Evacuation of large stones
within the gallbladder should also be performed. In general, the gallbladder
and its attachment to the intestines should be left alone.
Limey (Milk of Calcium) Bile and Porcelain
Gallbladder
Calcium
salts may be secreted into the lumen of the gallbladder in sufficient concentration
to produce calcium precipitation and diffuse, hazy opacification of bile or a
layering effect on plain abdominal roentgenography. This so-called limey bile,
or milk of calcium bile, is usually clinically innocuous, but cholecystectomy
is recommended because limey bile most often occurs in a hydropic gallbladder.
In the entity called porcelain gallbladder, calcium salt deposition
within the wall of a chronically inflamed gallbladder may be detected on the
plain abdominal film. Cholecystectomy is advised in all patients with porcelain
gallbladder because in a high percentage of cases this finding appears to be
associated with the development of carcinoma of the gallbladder.
![]() Treatment
Treatment
Medical Therapy
Although
surgical intervention remains the mainstay of therapy for acute cholecystitis
and its complications, a period of in-hospital stabilization may be required
before cholecystectomy. Oral intake is eliminated, nasogastric suction may be
indicated, and extracellular volume depletion and electrolyte abnormalities are
repaired. Meperidine or nonsteroidal antiinflammatory drugs (NSAIDs) are
usually employed for analgesia because they may produce less spasm of the
sphincter of Oddi than drugs such as morphine. Intravenous antibiotic therapy
is usually indicated in patients with severe acute cholecystitis even though
bacterial superinfection of bile may not have occurred in the early stages of
the inflammatory process. Postoperative complications of wound infection,
abscess formation, or sepsis are reduced in antibiotic-treated patients.
Effective antibiotics include ureidopenicillins, ampicillin, metronidazole, and
cephalosporins. Combination with an aminoglycoside or other antibiotics may be
considered in diabetic or debilitated patients and in those with signs of
gram-negative sepsis (Chap. 134).
Surgical Therapy
The
optimal timing of surgical intervention in patients with acute cholecystitis
depends on stabilization of the patient. The clear trend is toward earlier
surgery, and this is due in part to requirements for shorter hospital stays.
Urgent (emergency) cholecystectomy or cholecystostomy is probably appropriate
in most patients in whom a complication of acute cholecystitis such as empyema,
emphysematous cholecystitis, or perforation is suspected or confirmed. In
uncomplicated cases of acute cholecystitis, up to 30% of patients fail to
resolve their symptoms on appropriate medical therapy, and progression of the
attack or a supervening complication leads to the performance of early
operation (within 24 to 72 h). The technical complications of surgery are not
increased in patients undergoing early as opposed to delayed cholecystectomy. Delayed
surgical intervention is probably best reserved for (1) patients in whom the
overall medical condition imposes an unacceptable risk for early surgery and
(2) patients in whom the diagnosis of acute cholecystitis is in doubt. Early
cholecystectomy is the treatment of choice for most patients with acute
cholecystitis. Mortality figures for emergency cholecystectomy in most centers
approach 3%, while the mortality risk for elective or early cholecystectomy
approximates 0.5% in patients under age 60. Of course, the operative risks
increase with age-related diseases of other organ systems and with the presence
of long- or short-term complications of gallbladder disease. Seriously ill or
debilitated patients with cholecystitis may be managed with cholecystostomy and
tube drainage of the gallbladder. Elective cholecystectomy may then be done at
a later date.
Postcholecystectomy Complications
Early
complications following cholecystectomy include atelectasis and other pulmonary
disorders, abscess formation (often subphrenic), external or internal
hemorrhage, biliary-enteric fistula, and bile leaks. Jaundice may indicate
absorption of bile from an intraabdominal collection following a biliary leak
or mechanical obstruction of the CBD by retained calculi, intraductal blood
clots, or extrinsic compression. Routine performance of intraoperative
cholangiography during cholecystectomy has helped to reduce the incidence of
these early complications.
Overall,
cholecystectomy is a very successful operation that provides total or
near-total relief of preoperative symptoms in 75 to 90% of patients. The most
common cause of persistent postcholecystectomy symptoms is an overlooked
extrabiliary disorder (e.g., reflux esophagitis, peptic ulceration,
pancreatitis, or-most often-irritable bowel syndrome). In a small percentage of
patients, however, a disorder of the extrahepatic bile ducts may result in
persistent symptomatology. These so-called postcholecystectomy syndromes may be
due to (1) biliary strictures, (2) retained biliary calculi, (3) cystic duct
stump syndrome, (4) stenosis or dyskinesia of the sphincter of Oddi, or (5)
bile salt-induced diarrhea or gastritis.
Cystic Duct Stump Syndrome
In
the absence of cholangiographically demonstrable retained stones, symptoms
resembling biliary colic or cholecystitis in the postcholecystectomy patient
have frequently been attributed to disease in a long (>1 cm) cystic duct
remnant (cystic duct stump syndrome). Careful analysis, however, reveals that
postcholecystectomy complaints are attributable to other causes in almost all
patients in whom the symptom complex was originally thought to result from the
existence of a long cystic duct stump. Accordingly, considerable care should be
taken to investigate the possible role of other factors in the production of
postcholecystectomy symptoms before attributing them to cystic duct stump
syndrome.
Papillary dysfunction, papillary stenosis, spasm
of the sphincter of Oddi, and biliary dyskinesia
Symptoms
of biliary colic accompanied by signs of recurrent, intermittent biliary
obstruction may be produced by papillary stenosis, papillary dysfunction, spasm
of the sphincter of Oddi, and biliary dyskinesia. Papillary stenosis is thought
to result from acute or chronic inflammation of the papilla of Vater or from
glandular hyperplasia of the papillary segment. Five criteria have been used to
define papillary stenosis: (1) upper abdominal pain, usually RUQ or epigastric;
(2) abnormal liver tests; (3) dilatation of the common bile duct upon
endoscopic retrograde cholangiopancreatography (ERCP) examination; (4) delayed
(>45 min) drainage of contrast material from the duct; and (5) increased
basal pressure of the sphincter of Oddi, a finding that may be of only minor
significance. An alternative to ERCP is magnetic resonance cholangiography if
ERCP and/or biliary manometry are either unavailable or not feasible. In
patients with papillary stenosis, quantitative hepatobiliary scintigraphy has
revealed delayed transit from the common bile duct to the bowel, ductal
dilatation, and abnormal time-activity dynamics. This technique can also be
used before and after sphincterotomy to document improvement in biliary
emptying. Treatment consists of endoscopic or surgical sphincteroplasty to
ensure wide patency of the distal portions of both the bile and pancreatic
ducts. The greater the number of the preceding criteria present, the greater
the likelihood that a patient does have a degree of papillary stenosis
sufficient to justify correction. The factors usually considered as indications
for sphincterotomy include (1) prolonged duration of symptoms, (2) lack of
response to symptomatic treatment, (3) presence of severe disability, and (4)
the patient's choice of sphincterotomy over surgery (given a clear
understanding on his or her part of the risks involved in both procedures).
Criteria
for diagnosing dyskinesia of the sphincter of Oddi are even more controversial
than those for papillary stenosis. Proposed mechanisms include spasm of the
sphincter, denervation sensitivity resulting in hypertonicity, and
abnormalities of the sequencing or frequency rates of sphincteric contraction
waves. When thorough evaluation has failed to demonstrate another cause for the
pain, and when cholangiographic and manometric criteria suggest a diagnosis of
biliary dyskinesia, medical treatment with nitrites or anticholinergics to
attempt pharmacologic relaxation of the sphincter has been proposed. Endoscopic
biliary sphincterotomy (EBS) or surgical sphincteroplasty may be indicated in
patients who fail to respond to a 2- to 3-month trial of medical therapy,
especially if basal sphincter of Oddi pressures are elevated. EBS has become a
well-established procedure for removing bile duct stones and for other biliary
and pancreatic problems. Approximately 150,000 such procedures are performed
annually in the United States. Key findings in a recent study of EBS include:
(1) Dysfunction of the sphincter of Oddi was the most frequent patient-related
risk factor for complications; (2) pancreatitis was more frequent in young
patients; (3) difficulty in cannulating the bile duct and the use of
"precut" sphincterotomy were important technique-related risk factors
for complications; and (4) experience in the volume of procedures proved to be
important; endoscopists who perform more than one EBS per week had lower
complication rates than endoscopists who performed a smaller number of
procedures.
Bile Salt-Induced Diarrhea and Gastritis
Postcholecystectomy
patients may develop symptoms and signs of gastritis, which has been attributed
to duodenogastric reflux of bile. However, firm data linking an increased
incidence of bile gastritis with surgical removal of the gallbladder are
lacking. Cholecystectomy induces persistent changes in gut transit, and these
changes effect a noticeable modification of bowel habits. Cholecystectomy
shortens gut transit time by accelerating passage of the fecal bolus through
the colon with marked acceleration in the right colon, thus causing an increase
in colonic bile acid output and a shift in bile acid composition toward the
more diarrheagenic secondary bile acids. Diarrhea that is severe enough, i.e.,
three or more watery movements per day, can be classified as
postcholecystectomy diarrhea, and this occurs in 8 to 12% of patients undergoing
elective cholecystectomy. Treatment with a bile acid sequestering agent, such
as cholestyramine, is often effective in ameliorating troublesome diarrhea.
The Hyperplastic Cholecystoses
The
term hyperplastic cholecystoses is used to denote a group of disorders
of the gallbladder characterized by excessive proliferation of normal tissue
components.
Adenomyomatosis is characterized by a benign proliferation of
gallbladder surface epithelium with glandlike formations, extramural sinuses,
transverse strictures, and/or fundal nodule ("adenoma" or
"adenomyoma") formation. Outpouchings of mucosa termed Rokitansky-Aschoff
sinuses may be seen on oral cholecystography in conjunction with
hyperconcentration of contrast medium. Characteristic dimpled filling defects
also may be seen.
Cholesterolosis is characterized by abnormal deposition of
lipid, especially cholesterol esters, in the lamina propria of the gallbladder
wall. In its diffuse form ("strawberry gallbladder"), the gallbladder
mucosa is brick red and speckled with bright yellow flecks of lipid. The
localized form shows solitary or multiple "cholesterol polyps"
studding the gallbladder wall. Cholesterol stones of the gallbladder are found
in nearly half the cases. Cholecystectomy is indicated in both adenomyomatosis
and cholesterolosis when symptomatic or when cholelithiasis is present.
Diseases of the Bile Ducts
Congenital Anomalies
Biliary Atresia and Hypoplasia
Atretic
and hypoplastic lesions of the extrahepatic and major intrahepatic bile ducts
are the most common biliary anomalies of clinical relevance encountered in
infancy. The clinical picture is one of severe obstructive jaundice during the
first month of life, with pale stools. The diagnosis is confirmed by surgical
exploration with operative cholangiography. Approximately 10% of cases of
biliary atresia are treatable with roux-en-Y choledochojejunostomy, with the
Kasai procedure (hepatic portoenterostomy) being attempted in the remainder in
an effort to restore some bile flow. Most patients, even those having
successful biliary-enteric anastomoses, eventually develop chronic cholangitis,
extensive hepatic fibrosis, and portal hypertension.
Choledochal Cysts
Cystic
dilatation may involve the free portion of the CBD, i.e., choledochal cyst, or
may present as diverticulum formation in the intraduodenal segment. In the
latter situation, chronic reflux of pancreatic juice into the biliary tree can
produce inflammation and stenosis of the extrahepatic bile ducts leading to
cholangitis or biliary obstruction. Because the process may be gradual,
approximately 50% of patients present with onset of symptoms after age 10. The
diagnosis may be made by ultrasound, abdominal CT, or cholangiography. Only
one-third of patients show the classic triad of abdominal pain, jaundice, and
an abdominal mass. Ultrasonographic detection of a cyst separate from the
gallbladder should suggest the diagnosis of choledochal cyst, which can be
confirmed by demonstrating the entrance of extrahepatic bile ducts into the
cyst. Surgical treatment involves excision of the "cyst" and
biliary-enteric anastomosis. Patients with choledochal cysts are at increased
risk for the subsequent development of cholangiocarcinoma.
Congenital Biliary Ectasia
Cystic
dilatation of the intrahepatic bile ducts may involve either the major
intrahepatic radicles (Caroli's disease), the inter- and intralobular ducts
(congenital hepatic fibrosis), or both. In Caroli's disease, clinical
manifestations include recurrent cholangitis, abscess formation in and around
the affected ducts, and, sometimes, gallstone formation within portions of
ectatic intrahepatic biliary radicles. The CT scan and cholangiographic
patterns are usually diagnostic, and treatment with ongoing antibiotic therapy
is usually undertaken in an effort to limit the frequency and severity of
recurrent bouts of cholangitis. Progression to secondary biliary cirrhosis with
portal hypertension, amyloidosis, extrahepatic biliary obstruction,
cholangiocarcinoma, or recurrent episodes of sepsis with hepatic abscess
formation is common.
Choledocholithiasis
Pathophysiology and Clinical Manifestations
Passage
of gallstones into the CBD occurs in approximately 10 to 15% of patients with
cholelithiasis. The incidence of common duct stones increases with increasing
age of the patient, so that up to 25% of elderly patients may have calculi in
the common duct at the time of cholecystectomy. Undetected duct stones are left
behind in approximately 1 to 5% of cholecystectomy patients. The overwhelming
majority of bile duct stones are cholesterol or mixed stones formed in the
gallbladder, which then migrate into the extrahepatic biliary tree through the
cystic duct. Primary calculi arising de novo in the ducts are usually pigment
stones developing in patients with (1) chronic hemolytic diseases; (2)
hepatobiliary parasitism or chronic, recurrent cholangitis; (3) congenital
anomalies of the bile ducts (especially Caroli's disease); or (4) dilated,
sclerosed, or strictured ducts. Common duct stones may remain asymptomatic for
years, may pass spontaneously into the duodenum, or (most often) may present
with biliary colic or a complication.
Complications
Cholangitis
Cholangitis
may be acute or chronic, and symptoms result from inflammation, which usually
requires at least partial obstruction to the flow of bile. Bacteria are present
on bile culture in approximately 75% of patients with acute cholangitis early
in the symptomatic course. The characteristic presentation of acute cholangitis
involves biliary colic, jaundice, and spiking fevers with chills (Charcot's
triad). Blood cultures are frequently positive, and leukocytosis is typical. Nonsuppurative
acute cholangitis is most common and may respond relatively rapidly to
supportive measures and to treatment with antibiotics. In suppurative
acute cholangitis, however, the presence of pus under pressure in a completely
obstructed ductal system leads to symptoms of severe toxicity-mental confusion,
bacteremia, and septic shock. Response to antibiotics alone in this setting is
relatively poor, multiple hepatic abscesses are often present, and the
mortality rate approaches 100% unless prompt endoscopic or surgical relief of
the obstruction and drainage of infected bile are carried out. Endoscopic
management of bacterial cholangitis is as effective as surgical intervention.
ERCP with endoscopic sphincterotomy is safe and the preferred initial procedure
for both establishing a definitive diagnosis and providing effective therapy.
Obstructive Jaundice
Gradual
obstruction of the CBD over a period of weeks or months usually leads to
initial manifestations of jaundice or pruritus without associated symptoms of
biliary colic or cholangitis. Painless jaundice may occur in patients with
choledocholithiasis, but this manifestation is much more characteristic of
biliary obstruction secondary to malignancy of the head of the pancreas, bile
ducts, or ampulla of Vater.
In
patients whose obstruction is secondary to choledocholithiasis, associated
chronic calculous cholecystitis is very common, and the gallbladder in this
setting may be relatively indistensible. The absence of a palpable gallbladder
in most patients with biliary obstruction from duct stones is the basis for Courvoisier's
law, i.e., that the presence of a palpably enlarged gallbladder suggests
that the biliary obstruction is secondary to an underlying malignancy rather
than to calculous disease. Biliary obstruction causes progressive dilatation of
the intrahepatic bile ducts as intrabiliary pressures rise. Hepatic bile flow
is suppressed, and regurgitation of conjugated bilirubin into the bloodstream
leads to jaundice accompanied by dark urine (bilirubinuria) and light-colored
(acholic) stools.
CBD
stones should be suspected in any patient with cholecystitis whose serum
bilirubin level exceeds 85.5 ![]() mol/L
(5 mg/dL). The maximum bilirubin level is seldom over 256.5
mol/L
(5 mg/dL). The maximum bilirubin level is seldom over 256.5 ![]() mol/L
(15.0 mg/dL) in patients with choledocholithiasis unless concomitant hepatic
disease or another factor leading to marked hyperbilirubinemia exists. Serum
bilirubin levels of 342.0
mol/L
(15.0 mg/dL) in patients with choledocholithiasis unless concomitant hepatic
disease or another factor leading to marked hyperbilirubinemia exists. Serum
bilirubin levels of 342.0 ![]() mol/L
(20 mg/dL) or more should suggest the possibility of neoplastic obstruction.
The serum alkaline phosphatase level is almost always elevated in biliary
obstruction. A rise in alkaline phosphatase often precedes clinical jaundice
and may be the only abnormality in routine liver function tests. There may be a
two- to tenfold elevation of serum aminotransferases, especially in association
with acute obstruction. Following relief of the obstructing process, serum
aminotransferase elevations usually return rapidly to normal, while the serum
bilirubin level may take 1 to 2 weeks to return to normal. The alkaline
phosphatase level usually falls slowly, lagging behind the decrease in serum
bilirubin.
mol/L
(20 mg/dL) or more should suggest the possibility of neoplastic obstruction.
The serum alkaline phosphatase level is almost always elevated in biliary
obstruction. A rise in alkaline phosphatase often precedes clinical jaundice
and may be the only abnormality in routine liver function tests. There may be a
two- to tenfold elevation of serum aminotransferases, especially in association
with acute obstruction. Following relief of the obstructing process, serum
aminotransferase elevations usually return rapidly to normal, while the serum
bilirubin level may take 1 to 2 weeks to return to normal. The alkaline
phosphatase level usually falls slowly, lagging behind the decrease in serum
bilirubin.
Pancreatitis
The
most common associated entity discovered in patients with nonalcoholic acute
pancreatitis is biliary tract disease. Biochemical evidence of pancreatic
inflammation complicates acute cholecystitis in 15% of cases and
choledocholithiasis in over 30%, and the common factor appears to be the
passage of gallstones through the common duct. Coexisting pancreatitis should
be suspected in patients with symptoms of cholecystitis who develop (1) back
pain or pain to the left of the abdominal midline, (2) prolonged vomiting with
paralytic ileus, or (3) a pleural effusion, especially on the left side.
Surgical treatment of gallstone disease is usually associated with resolution
of the pancreatitis.
Secondary Biliary Cirrhosis
Secondary
biliary cirrhosis may complicate prolonged or intermittent duct obstruction
with or without recurrent cholangitis. Although this complication may be seen
in patients with choledocholithiasis, it is more common in cases of prolonged
obstruction from stricture or neoplasm. Once established, secondary biliary
cirrhosis may be progressive even after correction of the obstructing process,
and increasingly severe hepatic cirrhosis may lead to portal hypertension or to
hepatic failure and death. Prolonged biliary obstruction may also be associated
with clinically relevant deficiencies of the fat-soluble vitamins A, D, and K.
Diagnosis and Treatment
The
diagnosis of choledocholithiasis is usually made by cholangiography (Table
302-3), either preoperatively by ERCP or intraoperatively at the time of
cholecystectomy. As many as 15% of patients undergoing cholecystectomy will
prove to have CBD stones. With the advent of laparoscopic cholecystectomy, the
management of CBD stones in the presence of gallstones is gradually being
clarified. Preoperative ERCP with endoscopic papillotomy and stone extraction
is the preferred approach. It not only provides stone clearance but also
defines the anatomy of the biliary tree in relationship to the cystic duct.
ERCP is indicated in gallstone patients who have any of the following risk
factors: (1) a history of jaundice or pancreatitis, (2) abnormal tests of liver
function, and (3) ultrasonographic evidence of a dilated CBD or stones in the
duct. Alternatively, if intraoperative cholangiography reveals retained stones,
postoperative ERCP can be carried out. The need for preoperative ERCP is
expected to decrease further as laparoscopic techniques improve.
Table 302-3: Diagnostic Evaluation of the Bile
Ducts
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
The
widespread use of laparoscopic cholecystectomy and ERCP has decreased the
incidence of complicated biliary tract disease and the need for
choledocholithotomy and T-tube drainage of the bile ducts. EBS followed by
spontaneous passage or stone extraction is the treatment of choice in the
management of patients with common duct stones, especially in elderly or
poor-risk patients.
Trauma, Strictures, and Hemobilia
Benign
strictures of the extrahepatic bile ducts result from surgical trauma in
approximately 95% of cases and occur in about 1 in 500 cholecystectomies.
Strictures may present with bile leak or abscess formation in the immediate
postoperative period or with biliary obstruction or cholangitis as long as 2
years or more following the inciting trauma. The diagnosis is established by
percutaneous or endoscopic cholangiography. Endoscopic brushing of biliary
strictures is an effective way to establish the nature of the lesion and is
more accurate than bile cytology alone. When positive exfoliative cytology is
obtained, the diagnosis of a neoplastic stricture is established. This
procedure is especially important in patients with primary sclerosing
cholangitis who are predisposed to the development of cholangiocarcinomas.
Successful operative correction by a skillful surgeon with duct-to-bowel
anastomosis is usually possible, although mortality rates from surgical
complications, recurrent cholangitis, or secondary biliary cirrhosis are high.
Hemobilia
may follow traumatic or operative injury to the liver or bile ducts,
intraductal rupture of a hepatic abscess or aneurysm of the hepatic artery,
biliary or hepatic tumor hemorrhage, or mechanical complications of
choledocholithiasis or hepatobiliary parasitism. Diagnostic procedures such as
liver biopsy, percutaneous transhepatic cholangiography (PTHC), and transhepatic
biliary drainage catheter placement may also be complicated by hemobilia.
Patients often present with a classic triad of biliary colic, obstructive
jaundice, and melena or occult blood in the stools. The diagnosis is sometimes
made by cholangiographic evidence of blood clot in the biliary tree, but
selective angiographic verification may be required. Although minor episodes of
hemobilia may resolve without operative intervention, surgical ligation of the
bleeding vessel is frequently required.
Extrinsic Compression of the Bile Ducts
Partial
or complete biliary obstruction may sometimes be produced by extrinsic
compression of the ducts. The most common cause of this form of obstructive
jaundice is carcinoma of the head of the pancreas. Biliary obstruction may also
occur as a complication of either acute or chronic pancreatitis or involvement
of lymph nodes in the porta hepatis by lymphoma or metastatic carcinoma. The
latter should be distinguished from cholestasis resulting from massive
replacement of the liver by tumor.
Hepatobiliary Parasitism
Infestation
of the biliary tract by adult helminths or their ova may produce a chronic,
recurrent pyogenic cholangitis with or without multiple hepatic abscesses,
ductal stones, or biliary obstruction. This condition is relatively rare but
does occur in inhabitants of southern China and elsewhere in Southeast Asia.
The organisms most commonly involved are trematodes or flukes, including Clonorchis
sinensis, Opisthorchis viverrini or O. felineus, and Fasciola
hepatica. The biliary tract also may be involved by intraductal migration
of adult Ascaris lumbricoides from the duodenum or by intrabiliary
rupture of hydatid cysts of the liver produced by Echinococcus spp. The
diagnosis is made by cholangiography and the presence of characteristic ova on
stool examination. When obstruction is present, the treatment of choice is
laparotomy under antibiotic coverage, with common duct exploration and a
biliary drainage procedure. It should be emphasized that in the Far East, one
also sees cholangiohepatitis associated with pigment lithiasis, which may, in
fact, be more common than cholangitis due to parasites.
Sclerosing Cholangitis
Primary
or idiopathic sclerosing cholangitis is characterized by a progressive,
inflammatory, sclerosing, and obliterative process affecting the extrahepatic
and/or the intrahepatic bile ducts. The disorder occurs in about 70% in
association with inflammatory bowel disease, especially ulcerative colitis. It
may also be associated (albeit rarely) with multifocal fibrosclerosis syndromes
such as retroperitoneal, mediastinal, and/or periureteral fibrosis; Riedel's
struma; or pseudotumor of the orbit. In patients with AIDS,
cholangiopancreatography may demonstrate a broad range of biliary tract changes
as well as pancreatic duct obstruction and occasionally pancreatitis (Chap.
309). Further, biliary tract lesions in AIDS include infection and
cholangiopancreatographic changes similar to primary sclerosing cholangitis.
Changes noted include: (1) diffuse involvement of intrahepatic bile ducts
alone, (2) involvement of both intra- and extrahepatic bile ducts, (3)
ampullary stenosis, (4) stricture of the intrapancreatic portion of the common
bile duct, and (5) pancreatic duct involvement. Associated infectious organisms
include Cryptosporidium, Mycobacterium avium-intracellulare,
cytomegalovirus, Microsporidia, and Isospora. In addition,
acalculous cholecystitis occurs in up to 10% of patients. ERCP sphincterotomy,
while not without risk, provides significant pain reduction in patients with
AIDS-associated papillary stenosis. Secondary sclerosing cholangitis may occur
as a long-term complication of choledocholithiasis, cholangiocarcinoma,
operative or traumatic biliary injury, or contiguous inflammatory processes.
Patients
with primary sclerosing cholangitis often present with signs and symptoms of
chronic or intermittent biliary obstruction: jaundice, pruritus, RUQ abdominal
pain, or acute cholangitis. Late in the course, complete biliary obstruction,
secondary biliary cirrhosis, hepatic failure, or portal hypertension with
bleeding varices may occur. The diagnosis is usually established by finding
multifocal, diffusely distributed strictures with intervening segments of
normal or dilated ducts, producing a beaded appearance on cholangiography (Fig.
302-2D). The cholangiographic technique of choice in suspected cases is
ERCP, since intrahepatic ductal involvement may make PTHC difficult. When a
diagnosis of sclerosing cholangitis has been established, a search for
associated diseases, especially for chronic inflammatory bowel disease, should
be carried out.
A
recent study describes the natural history and outcome for 305 patients of
Swedish descent with primary sclerosing cholangitis; 134 (44%) of the patients
were asymptomatic at the time of diagnosis and, not surprisingly, had a
significantly higher survival rate with a median follow-up time of 63 months.
The independent predictors of a bad prognosis were age, serum bilirubin
concentration, and liver histologic changes. Cholangiocarcinoma was found in 24
patients (8%). Inflammatory bowel disease was closely associated with primary
sclerosing cholangitis and had a prevalence of 81% in this study population.
![]() Treatment
Treatment
Therapy
with cholestyramine may help control symptoms of pruritus, and antibiotics are
useful when cholangitis complicates the clinical picture. Vitamin D and calcium
supplementation may help prevent the loss of bone mass frequently seen in
patients with chronic cholestasis. Glucocorticoids, methotrexate, and
cyclosporine have not been shown to be efficacious. UDCA improves serum liver
tests, but an effect on survival has not been documented. In cases where
complete or high-grade biliary obstruction (dominant strictures) has occurred,
balloon dilatation, stenting, or (rarely) surgical intervention may be
appropriate. Efforts at biliary-enteric anastomosis or stent placement may,
however, be complicated by recurrent cholangitis and further progression of the
stenosing process. The role of colectomy in patients with sclerosing
cholangitis complicating chronic ulcerative colitis is uncertain. The prognosis
is unfavorable, with a median survival of 9 to 12 years following the
diagnosis, regardless of therapy. Four variables (age, serum bilirubin level,
histologic stage, and splenomegaly) predict survival in patients with primary
sclerosing cholangitis and serve as the basis for a risk score. Primary
sclerosing cholangitis is one of the most common indications for liver
transplantation.
Gallbladder Polyps
In
two large studies involving 627 and 3147 patients, the prevalence of
gallbladder polyps was 6.7 and 6.9%, respectively, with a marked male predominance.
Few significant changes occurred over a 5-year period in asymptomatic patients
in whom gallbladder polyps <10 mm in diameter were found. If polyps >10
mm are present and show rapid growth, cholecystectomy should be considered.